Cushing's Disease in Cavalier King Charles Spaniels
-
 What
It Is
What
It Is - Symptoms
- Diagnosis
- Related Disorders
- Treatment
- Breeders' Responsibilities
- Research News
- Related Links
- Veterinary Resources
The cavalier King Charles spaniel is at increased risk for Cushing's disease, also known as Cushing's syndrome or hyperadrenocorticism (HAC) or spontaneous hypercortisolism (HC). It is a serious, genetic disorder which produces excess cortisol, a natural steroidal hormone, from the adrenal glands and/or pituitary gland. If not promptly treated, it can lead to life-threatening disorders. (Photo is courtesy of The Cavalier Alliance.)
RETURN TO TOP
What It Is
The adrenal glands produce hormones which help regulate weight, mineral balance, the structure of connective tissue, some white blood cell production, and skin health. The pituitary gland controls the adrenals, and it may be the initiator of the disorder.
Cushing's disease is caused by either an adrenal cortical tumor (a tumor of the cortisol-producing cells of the adrenal gland) or pituitary tumors (which produce excessive amounts of ACTH -- adrenocorticotrophic hormone, the hormone which causes the adrenal glands to produce cortisol), with the result that an excess of cortisol is released in the cavalier's body. These tumors may or may not be cancerous. This form of Cushing's diseaw also is referred to as Typical Cushing's.
Cushing's disease also may occur due to the administration of glucocorticords such as prednisone, a steroid, in some dogs. This is called iatrogenic Cushing's disease, meaning that it is unintentionally induced as a side effect to medical treatment. ("Iatrogenic" is veterinary-ese for "the vet screwed up!")
Other forms of Cushing's disease are (a) Atypical Cushing's, in which cortisol levels remain normal and no tumors are produced, but the dog's sex hormones may be elevated, and it has symptoms similar to Typical Cushing's; and (b) Meal-Induced Cushing's, in which the dog's cortisol levels may spike after meals.
Addison's disease is hypoadrenocorticism, the opposite of Cushing's disease.
RETURN TO TOP
Symptoms
Symptoms include:
• Excessive drinking (polydipsia)
• Excessive and urination (polyuria)
• Increased appetite (polyphagia)
• Panting
• Symmetrical hair loss (alopecia), particulaarly along the chest, flanks, and tail
• Hard, calcified lumps in the skin (calcinosis cutis)
• Skin discoloration, particularly on the abdomen
• Lethargy
• Muscle weakness
• Susceptibility to skin and urinary infections.
Victims also develop bulging, sagging bellies, due to decreased muscle strength and the redistribution of fat from body storage areas to the abdomen.
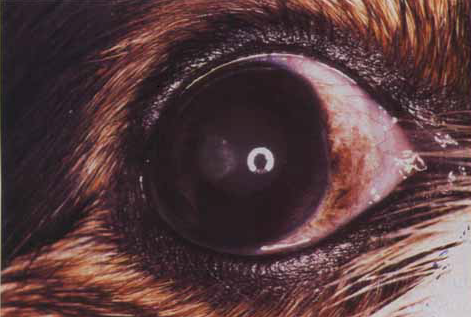 In
a 1993 report, Dr. Shiela Crispin found that, especially in the
cavalier King Charles spaniel, crystalline stromal dystrophy due to
hyperlipoproteinaemmia (raised HDL, LDL, and VLDL) is an ocular
manifestation of Cushing's syndrome. (The photo at right, from Dr.
Crispin's 1993 report, shows the eye of a cavalier with crystalline
stromal dystrophy secondary to hyperlipoproteinaemia associated with
Cushing’s syndome. The right eye is shown and the lipid is situated
immediately lateral to the camera flash.)
In
a 1993 report, Dr. Shiela Crispin found that, especially in the
cavalier King Charles spaniel, crystalline stromal dystrophy due to
hyperlipoproteinaemmia (raised HDL, LDL, and VLDL) is an ocular
manifestation of Cushing's syndrome. (The photo at right, from Dr.
Crispin's 1993 report, shows the eye of a cavalier with crystalline
stromal dystrophy secondary to hyperlipoproteinaemia associated with
Cushing’s syndome. The right eye is shown and the lipid is situated
immediately lateral to the camera flash.)
RETURN TO TOP
Diagnosis
Cushing's disease can be diagnosed by laboratory tests of blood and urine, including a urine cortisol / creatinine ratio test (UCCR), an ACTH stimulation test, and low-dose dexamethasone suppression test (LDDST). Once diagnosed, tests can also determine if it is caused by pituitary gland tumors or an adrenal gland tumor, including ultrasound.
 A
March 2018 article points out about the ACTH stimulation test and
the LDDST that:
A
March 2018 article points out about the ACTH stimulation test and
the LDDST that:
"Neither of these tests is wholly accurate in confirming the diagnosis in animals with HAC, nor in excluding it in dogs presenting with non-adrenal illness (NAI). The ACTH stimulation test reportedly has low sensitivity but high specificity for diagnosis of HAC and performs particularly poorly in dogs with functional adrenal tumors (AT). The sensitivity and specificity of the LDDST for diagnosis of HAC are reported as being 85%-100% and 44%-73%, respectively. Because the LDDST lacks specificity, it is only recommended in dogs in which there is a strong indication to pursue a diagnosis of HAC to maximize the positive predictive value (PPV) of the test. Where specifically evaluated, the PPV of the LDDST has been reported to be as low as 38% and as high as 92%."
In two 2013 studies of dog hair specimens, both panels of researchers found that the level of cortisol in dogs' hair is much higher when the dogs have hyperadrenocorticism. In the first 2013 report, a team of Austrian researchers stated: "Measuring cortisol in hair is so much easier and less painful to the animal than other tests for the disease and we think it has real promise for use as a rapid and non-invasive method to diagnose hyperadrenocorticism." In the second 2013 study, Italian researchers found that hair cortisol concentrations are higher in dogs with Cushings, compared to sick control dogs and healthy dogs. They stated: "It is a noninvasive technique that should be further investigated as a possible diagnostic procedure for the diagnosis of HC [hypercortisolism] in dogs."
In an April 2019 article reviewing diagnosis and treatment of 219 dogs diagnosed with hyperadrenocorticism, the authors found that ACTH stimulation was the predominate test performed, and that differentiation between pituitary and adrenal disase was infrequently performed, contrary to current expert recommendations.
RETURN TO TOP
Related Disorders
Dogs with Cushing's disease are predisposed to other diseases, such as diabetes mellitus, urinary tract infections, kidney disease, high blood pressure, and pancreatitis.
RETURN TO TOP
Treatment
Left untreated, Cushing's disease can lead to life-threatening disorders such as diabetes, congestive heart failure, and liver and kidney failure, and to chronic problems of hypothyroidism, and infections of the skin, ears, gums, eyes, or bladder.
The goal of medication is to reduce the levels of cortisol. Drug therapies include:
• trilostane (Modrenal, Vetoryl)
• Mitotane (lysodren)
• ketoconazole (Nizoral)
• anipryl (Deprenyl, Eldepryl, Selegiline)
Trilostane (Modrenal, Vetoryl) is a synthetic steroid which the FDA has approved for the treatment of canine Cushings. It reduces synthesis of cortisol, aldosterone, and adrenal androgens, and the effects appear to be reversible and dose dependent in most patients. Oral trilostane is rapidly absorbed, and absorption is enhanced when administered with food. It reportedly can cause serum potassium levels to become elevated. Therefore, trilostane should be used with caution with ACE-inhibitors and spironolactone, drugs customarily prescribed for dogs in advanced stages of mitral valve disease. See this September 2014 article. Also, Plumb's warns that "Trilostane is a hazardouse drug. Do not open capsules or attempt to divide capsules into smaller sizes."
Mitotane (lysodren) is not FDA-approved. It is an adrenocorticolytic agent, and its effects may not be reversible. There are conflicting reports regarding whether mitotane may induce hypoadrenocorticism (Addison's disease) in cavaliers. Compare this 2005 report with this 2008 powerpoint presentation, both submitted by Michael E. Herrtage. Because of the critical nature of mitotane's induction phase and the potential serious side effects of therapy, it must be carefully monitored.
Ketoconazole (Nizoral) an antifungal, inhibits P-glycoprotein, the important drug efflux transporter in the GI tract, kidney(s), biliary tree, and brain. Therefore, ketoconazole can decrease the bioavailability and/or clearance of many drugs. For example, ketoconazole increases blood cyclosporine concentrations, which can allow lower therapeutic doses of cyclosporine. Ketoconazole also can as much as double ivermectin exposure in dogs. See this June 2013 report.
Surgery can remove an adrenal cortical tumor that has not spread to other areas of the body. However, about half of adrenal tumors are malignant and may have already spread. Removing the pituitary gland (hypophysectomy) is much more complex and less often performed. Otherwise, pituitary Cushing's disease cannot be cured, but the treatment can prolong the cavalier's quality of life, but not to increase the lifespan. Following these surgeries, the patients will need hormonal replacements.
Radiation therapy is another option for treating Cushing's which is not responsive to other modalities of treatment.
Successful homeopathic therapies have included a mixture of ACTH and Quercus robur. In a January 2001 article, the researcher reports an 80% success rate in treating 18 Cushing-affected dogs with this homeopathic remedy. Others include melatonin, glandulars, and acupuncture.
RETURN TO TOP
Breeders' Responsibilities
 Cavaliers diagnosed with Cushing's, or otherwise determined to be
pre-disposed to it, should not be bred. Any littermates of breeding stock having
Cushing's disease should be taken into consideration. The
Canine Inherited
Disorders Database advises to breed only dogs from
families with no history of the disorder. Any cavalier King Charles spaniel
intended to be bred should be blood tested for Cushing's disease at least
annually, the closer the examination to the breeding the better.
Cavaliers diagnosed with Cushing's, or otherwise determined to be
pre-disposed to it, should not be bred. Any littermates of breeding stock having
Cushing's disease should be taken into consideration. The
Canine Inherited
Disorders Database advises to breed only dogs from
families with no history of the disorder. Any cavalier King Charles spaniel
intended to be bred should be blood tested for Cushing's disease at least
annually, the closer the examination to the breeding the better.
RETURN TO TOP
Research News
December 2021: Cavaliers ranked 9th in prevalence of Cushing's syndrome in UK study of 905,544 dogs. In a December 2021 article by UK researchers I. Schofield, D. C. Brodbelt, S. J. M. Niessen, D. B. Church, R. F. Geddes, D. G. O'Neill, the 2016 medical records of 905,544 were examined for the frequency of naturally occurring Cushing's syndrome. The investigators report finding 970 pre-existing and 557 new incident cases, making the species-wide prevalence of 0.17%. Cavalier King Charles spaniels ranked 9th among all breeds in prevalence of the disease, following border terriers and miniature schnauzers at the top of the llist.
 January
2019:
Cavaliers and neutered females were found at high risk of
developing Cushing's disease in Italian study. In a
January 2019 study by Italian researchers (Gaia Carotenuto, Eleonora
Malerba, Costanza Dolfini, Francesca Brugnoli, Pasquale Giannuzzi,
Giovanni Semprini, Paolo Tosolin, Federico Fracassi [right]) of
21,281 dogs of 31 different breeds, cavalier King Charles spaniels
ranked third, behind standard schnauzers and fox terriers in being at
risk of developing Cushing's disease (spontaneous hypercortisolism).
That study also found that neutered female dogs were at the highest risk
for spontaneous hypercortisolism.
January
2019:
Cavaliers and neutered females were found at high risk of
developing Cushing's disease in Italian study. In a
January 2019 study by Italian researchers (Gaia Carotenuto, Eleonora
Malerba, Costanza Dolfini, Francesca Brugnoli, Pasquale Giannuzzi,
Giovanni Semprini, Paolo Tosolin, Federico Fracassi [right]) of
21,281 dogs of 31 different breeds, cavalier King Charles spaniels
ranked third, behind standard schnauzers and fox terriers in being at
risk of developing Cushing's disease (spontaneous hypercortisolism).
That study also found that neutered female dogs were at the highest risk
for spontaneous hypercortisolism.
January 2016:
Researchers find significant breed variations in cortisol and
other concentrations in healthy dogs.
 In a
January 2016 article in which 531 healthy dogs of 9 breeds,
including 34 cavalier King Charles spaniels, were tested to measure
their circulating concentrations of plasma endothelin-1 (ET-1), plasma
renin activity, and serum cortisol, the researchers (K. Höglund
[right], A.-S. Lequarré, I. Ljungvall, K. Mc Entee, A.-C.
Merveille, M. Wiberg, V. Gouni, J. Lundgren Willesen, S. Hanås, G. Wess,
L. Mejer Sørensen, L. Tiret M. Kierczak, S.K.G. Forsberg, E. Seppälä, K.
Lindblad-Toh, H. Lohi, V. Chetboul, M. Fredholm, J. Häggström) found significant
breed differences in all three categories. Newfoundlands had highest
median ET-1 concentration, 3 times higher than cavaliers, Doberman
pinschers, and Dachshunds. Median renin activity was highest in
Dachshunds, twice the median value in Newfoundlands and boxers. Median
cortisol concentration was highest in Finnish Lapphunds, almost 3 times
higher than in boxers. They concluded that breed variation might be
important to take into consideration when interpreting test results in
clinical studies.
In a
January 2016 article in which 531 healthy dogs of 9 breeds,
including 34 cavalier King Charles spaniels, were tested to measure
their circulating concentrations of plasma endothelin-1 (ET-1), plasma
renin activity, and serum cortisol, the researchers (K. Höglund
[right], A.-S. Lequarré, I. Ljungvall, K. Mc Entee, A.-C.
Merveille, M. Wiberg, V. Gouni, J. Lundgren Willesen, S. Hanås, G. Wess,
L. Mejer Sørensen, L. Tiret M. Kierczak, S.K.G. Forsberg, E. Seppälä, K.
Lindblad-Toh, H. Lohi, V. Chetboul, M. Fredholm, J. Häggström) found significant
breed differences in all three categories. Newfoundlands had highest
median ET-1 concentration, 3 times higher than cavaliers, Doberman
pinschers, and Dachshunds. Median renin activity was highest in
Dachshunds, twice the median value in Newfoundlands and boxers. Median
cortisol concentration was highest in Finnish Lapphunds, almost 3 times
higher than in boxers. They concluded that breed variation might be
important to take into consideration when interpreting test results in
clinical studies.
November 2013:
ACVIM issues a Consensus Statement on diagnosis of spontaneous canine
 hyperadrenocorticism.
The ACVIM has published a
Consensus
Statement on the diagnosis of Cushing's Disease (hyperadrenocorticism). In
summary, it states:
hyperadrenocorticism.
The ACVIM has published a
Consensus
Statement on the diagnosis of Cushing's Disease (hyperadrenocorticism). In
summary, it states:
"Endocrine tests should be performed only when clinical signs consistent with HAC are present. None of the biochemical screening or differentiating tests for hyperadrenocorticism are perfect. Imaging can also play a role. Awareness of hyperadrenocorticism has heightened over time. Thus, case presentation is more subtle. Due to the changes in manifestations as well as test technology the Panel believes that references ranges should be reestablished. The role of cortisol precursors and sex hormones in causing a syndrome of occult hyperadrenocorticism remains unclear."
July 2013: Italian researchers also conclude that hair cortisol concentrations are higher in dogs with Cushing's. A panel of Italian researchers compared corticsol concentrations in the hair of dogs with and without hypercortisolism (Cushing's disease). In their July 2013 study, they found that hair cortisol concentrations are higher in dogs with Cushings, compared to sick control dogs and healthy dogs. They state: "It is a noninvasive technique that should be further investigated as a possible diagnostic procedure for the diagnosis of HC [hypercortisolism] in dogs."
 July
2013:
Austrian researchers find dog hair samples indicate higher levels of cortisol
in dogs with Cushing's disease. In an
August 2013 study by
researchers (Claudia Ouschan [right], Alexandra Kuchar, Erich Möst) at
the University of Veterinary Medicine, Vienna, they found that the level of
cortisol in dogs' hair is much higher when the dogs have hyperadrenocorticism.
They stated: "Measuring cortisol in hair is so much easier and less painful to
the animal than other tests for the disease and we think it has real promise for
use as a rapid and non-invasive method to diagnose hyperadrenocorticism."
July
2013:
Austrian researchers find dog hair samples indicate higher levels of cortisol
in dogs with Cushing's disease. In an
August 2013 study by
researchers (Claudia Ouschan [right], Alexandra Kuchar, Erich Möst) at
the University of Veterinary Medicine, Vienna, they found that the level of
cortisol in dogs' hair is much higher when the dogs have hyperadrenocorticism.
They stated: "Measuring cortisol in hair is so much easier and less painful to
the animal than other tests for the disease and we think it has real promise for
use as a rapid and non-invasive method to diagnose hyperadrenocorticism."
July 2012: Texas A&M researchers find compounded trilostane may be defective. In a July 2012 report, a team of researchers from Texas A&M University (Audrey K. Cook, Cornelia D. Nieuwoudt, and Susan L. Longhofer) evaluated 96 batches of compounded trilostane products from eight pharmacies. They found a wide variablity in actual drug content, compared to the labels' claims. They determined that the defective products may compromise effective management of patients being treated for hyperadrenocorticism.
RETURN TO TOP
Related Links
RETURN TO TOP
Veterinary Resources
Ocular manifestations of hyperlipoproteinaemia. S. M. Crispin. J.Small Animal Prac.;Oct. 1993;34(10):500-506. Quote: "The ocular manifestations of hyperlipoproteinaemia include visible lipaemia of ocular blood vessels, corneal opacities, lipaemic aqueous and gross infiltration of the globe itself which is easiest to observe in the peripheral cornea and uveal tract. Both primary and secondary hyperlipoproteinaemia may produce ocular signs and the ocular appearance can be characteristic of the underlying lipoprotein disorder. ... Crystalline stromal dystrophy in a Cavalier King Charles spaniel with secondary hyperlipoproteinaemia associated with Cushing’s syndome. ... Crystalline stromal dystrophy [due to] Hyperlipoproteinaemmia (raised HDL, LDL, and VLDL) [is an] ocular manifestation [of the] clinical disorder Cushing's syndrome especially in the Cavalier King Charles Spaniel.
Control of Canine Genetic Diseases. Padgett, G.A., Howell Book House 1998, pp. 198-199, 222.
Aortic and iliac thrombosis in six dogs. A. Boswood C. R. Lamb R. N. White. J. Sm. Anim. Pract. March 2000;41(2):109-114. Quote: Six dogs [including a cavalier King Charles spaniel] had signs of pelvic limb weakness, pain and collapse as a result of occlusion of the distal aorta and/or the iliac arteries by a thrombus. Antemortem diagnosis was made on the basis of clinical signs, angiography and ultrasonography. Five dogs had concurrent disease that probably predisposed to thrombosis, including hyperadrenocorticism (three dogs [including the cavalier]), neoplasia and cardiac disease. Two dogs [including the cavalier] died shortly after the episode of thrombosis. Dogs that survived the acute episode received aspirin in an attempt to prevent thrombosis occurring again and all regained pelvic limb function. For dogs that survived longer than one month after the acute episode, repeat thrombosis was uncommon; hence the prognosis was related to the underlying disease. Aortic and iliac thrombosis in dogs is an uncommon condition that usually arises secondarily to a predisposing disease process; it carries a more favourable prognosis than feline aortic thromboembolism. ... The dog with iatrogenic HAC [hyperadrenocorticism] was a Cavalier King Charles spaniel. ... The Cavalier reported in the present study, however, demonstrated marked clinical signs of ataxia, knuckling and paresis. ... Postmortem examination revealed the presence of a thrombus in the distal aorta at the site of bifurcation. The aortic thrombus appeared recent with no evidence of organisation. Within the iliac artery there was marked endothelial mineralisation and the thrombus was adherent to the wall at several points.
Cushing’s Disease: a new approach to therapy in equine and canine patients. M Elliott. Brit. Homoeopathic J. January 2001;90(1):33-36. Quote: Forty-one cases of Cushing's Disease affecting both equine and canine patients were treated with an identical mixture of two homeopathically prepared remedies (ACTH 30c and Quercus robur 30c), and the clinical improvements seen in the cases assessed. Homeopathy has been described as a medicine that can only be prescribed on the basis of individual symptoms shown, fitting the remedy to the patient, not the disease. The aim of this study was to define whether a standardised approach, using homeopathically prepared remedies, was a valid system of therapy for this disease, and if so, whether results were repeatable between species. The overall success rate for the therapy was 80% and results were broadly similar between the two species, indicating that homeopathy lends itself to the treatment of Cushing's Disease, and also to both cohort studies and group medicine.
A Comparison of the Survival Times of Dogs Treated with Mitotaneor Trilostane for Pituitary-Dependent Hyperadrenocorticism. E.N. Barker, S. Campbell, A.J. Tebb, R. Neiger, M.E. Herrtage, S.W.J. Reid, and I.K. Ramsey. J Vet Intern Med; 2005;19:810–815. Quote: "The survival times of 148 dogs [including 6 cavalier King Charles spaniels] treated for pituitary-dependent hyperadrenocorticism were studied using clinical records from 3UK veterinary centers between 1998 and 2003. Of these animals, 123 (83.1%) were treated with trilostane, while 25 (16.9%) weretreated with mitotane. Treatment groups were compared using t-tests and analysis of variance (or their nonparametric equivalents)and chi-square tests. Survival data were analyzed using Kaplan-Meier survival plots and Cox proportional hazard methods. Therewas no significant difference between the population attributes from each center or between treatment groups. The median survival time for animals treated with trilostane was 662 days (range 8–1,971) and for mitotane it was 708 days (range 33–1,399). There were no significant differences between the survival times for animals treated with trilostane and those treated with mitotane. In the multivariable model (including drug, center, breed group, weight, diagnostic group, and age at diagnosis), only age at diagnosis and weight were significantly negatively associated with survival. Importantly, there was no significant effect of drug choice on survival."
Diagnosis and Management of Hypoadrenocorticism. Michael E. Herrtage. 2008. Quote: "Mitotane-induced hypoadrenocorticism: breed incidence: higher in Scottish terrier, Cavalier King Charles spaniel, Cocker spaniel, Springer spaniel, and Yorkshire terrier. Age range: range 4 - 10 years; mean 8.4 years."
Use of Computed Tomography Adrenal Gland Measurement for Differentiating ACTH Dependence from ACTH Independence in 64 Dogs with Hyperadenocorticism. M.I. Rodríguez Piñeiro, P. de Fornel-Thibaud, G. Benchekroun, F. Garnier, C. Maurey-Guenec, F. Delisle, D. Rosenberg. J Vet Int Med Sept 2011; 25(5):1066-1074. Quote: "The measurement of adrenal gland size on computed tomography (CT) scan has been proposed for the etiological diagnosis of hyperadrenocorticism (HAC) in dogs. Symmetric adrenal glands are considered to provide evidence for ACTH-dependent hyperadrenocorticism (ADHAC), whereas asymmetry suggests ACTH-independent hyperadrenocorticism (AIHAC). However, there are currently no validated criteria for such differentiation. Objective: The aim of this retrospective study was to compare various adrenal CT scan measurements and the derived ratios in ADHAC and AIHAC cases, and to validate criteria for distinguishing between these conditions in a large cohort of dogs. Results: An overlap was systematically observed between the AIHAC and ADHAC groups for all measurements tested. Overlaps also were observed for ratios tested. For the maximum adrenal diameter ratio derived from reformatted images (rADR), only 1/18 AIHAC dogs had a rADR within the range for ADHAC. For a threshold of 2.08, the 95% confidence intervals for estimated sensitivity and specificity extended from 0.815 to 1.000 and from 0.885 to 0.999, respectively, for AIHAC diagnosis. Conclusion and Clinical Importance: Measurements from cross-sectional or reformatted CT scans are of little use for determining the origin of HAC. However, rADR appears to distinguish accurately between ADHAC and AIHAC, with a rADR > 2.08 highly suggestive of AIHAC."
Pharmaceutical Evaluation of Compounded Trilostane Products. Audrey K. Cook, Cornelia D. Nieuwoudt, and Susan L. Longhofer. J Am Anim Hosp Assoc. Jul/Aug 2012;48(4):228-233. Quote: "Compounded trilostane capsules (15 mg, 45 mg, or 100 mg) were purchased from eight pharmacies and assayed for content and dissolution characteristics. Capsules made in-house containing either inert material or 15 mg of the licensed product and proprietary capsules (30 mg and 60 mg) served as controls. Findings were compared with regulatory specifications for the licensed product. Altogether, 96 batches of compounded trilostane and 16 control batches underwent analysis. In total, 36 of 96 (38%) compounded batches were below the acceptance criteria for content. The average percentage label claim (% LC) for each batch ranged from 39% to 152.6% (mean, 97.0%). The range of average % LC for the controls was 96.1–99.6% (mean, 97.7%). The variance in content of the purchased compounded products was substantially greater than for the controls (234.65 versus 1.27; P<0.0001). All control batches exceeded the acceptance criteria for dissolution, but 19 of 96 batches (20%) of purchased compounded products did not. Mean percent dissolution for the purchased compounded products was lower than for controls (75.96% versus 85.12%; P=0.013). These findings indicate that trilostane content of compounded capsules may vary from the prescribed strength, and dissolution characteristics may not match those of the licensed product. The use of compounded trilostane products may therefore negatively impact the management of dogs with hyperadrenocorticism."
Applied Dermatology: Old or New? A Comparison of Mitotane and Trilostane for the Management of Hyperadrenocorticism. Joel D. Griffies. Compendium. May 2013; 35(5). Quote: "Hyperadrenocorticism (HAC) is a common endocrinopathy in dogs. With better recognition of the disease, more cases are being presented to clinicians for management. Mitotane, a 3- to 4-decade-old therapy, remains a viable and useful option for management of this disease. Thorough education and understanding of the drug are important, however, as the learning curve of how to manage its effects can be significant. Trilostane, a newer option for management of HAC, offers a simplified protocol and, often, smoother and faster control of the disease. ... Both mitotane and trilostane are useful tools in the management of an often insidious chronic disease. While both have pros and cons, the clinician’s comfort level, experience, and understanding of each drug are probably the most important features in deciding which to choose. With proper drug therapy, patient follow-up, and client communication, successful management of HAC can result in significantly improved quality of life for the patient and the owner."
Drug Interactions in Polypharmacy. Lauren A. Trepanier. Clinician's Brief. June 2013:23-26.
Measurement of cortisol in dog hair: a noninvasive tool for the diagnosis of hypercortisolism. Claudia Ouschan, Alexandra Kuchar, Erich Möst. Vet.Dermatology. August 2013;24(4):428-e94. Summary: "As the hormones are known to be present in hair, at least in humans, Ouschan reasoned that measuring glucocorticoid concentrations in dog hair might represent a way of diagnosing Cushing’s disease without causing the animals unnecessary distress. She thus compared the levels of cortisol, corticosterone and cortisone in the hair of twelve dogs with hyperadrenocorticism and ten healthy dogs. The results were striking: all three hormones were found at far higher levels in the hair of dogs with Cushing’s disease than in the control group, with the increase in cortisol particularly pronounced. The importance of the finding is clear. As Ouschan says, 'we have shown that the level of cortisol in dogs’ hair is much higher when the animals have hyperadrenocorticism. Measuring cortisol in hair is so much easier and less painful to the animal than other tests for the disease and we think it has real promise for use as a rapid and non-invasive method to diagnose hyperadrenocorticism.'"
Evaluation of Hair Cortisol in the Diagnosis of Hypercortisolism in Dogs. S. Corradini, P.A. Accorsi, A. Boari, V. Beghelli, M. Mattioli, P. Famigli-Bergamini, F. Fracassi. J.Vet.Int.Med. July 2013. Quote: "Background: Measurement of hair cortisol is a noninvasive technique used for several purposes in humans and in animals. Objectives: To measure hair cortisol concentrations (HCC) in dogs with spontaneous hypercortisolism (HC) and determine whether it can represent a useful diagnostic test for this syndrome. Animals: Twenty-two dogs with spontaneous HC before treatment, 28 sick control dogs (SCD), and 40 healthy dogs. Methods: In this prospective, observational clinical study, the HCC was measured by an RIA assay after extraction in HC dogs, in dogs with other chronic diseases, and in healthy dogs. The diagnostic accuracy of HCC was evaluated by subjecting data from dogs with HC and dogs with other chronic diseases to receiver operating characteristic (ROC) curve analysis. Results: Median (range) cortisol concentration in dogs with HC was 4.53 pg/mg (0.32–74.62 pg/mg) and was significantly higher than in SCD (1.49 pg/mg, 0.13–14.19 pg/mg) and healthy dogs (1.28 pg/mg, 0.34–5.38 pg/mg). Within the 3 groups, there was a large overlap of HCC. The area under the ROC curve was 0.80 (95% CI: 0.67–0.92). A cut-off value of HCC of 1.93 pg/mg revealed 91% sensitivity and 61% specificity to diagnose HC. Conclusions and Clinical Importance: Hair cortisol concentrations are higher in dogs with HC compared to SCD and healthy dogs. It is a noninvasive technique that should be further investigated as a possible diagnostic procedure for the diagnosis of HC in dogs."
Diagnosis of Spontaneous Canine Hyperadrenocorticism: 2012 ACVIM Consensus Statement (Small Animal). E.N. Behrend, H.S. Kooistra, R. Nelson, C.E. Reusch and J.C. Scott-Moncrieff. J.Vet.Int.Med. Nov. 2013;27(6):1292-1304. Quote: "This report offers a consensus opinion on the diagnosis of spontaneous canine hyperadrenocorticism. The possibility that a patient has hyperadrenocorticism is based on the history and physical examination. Endocrine tests should be performed only when clinical signs consistent with HAC are present. None of the biochemical screening or differentiating tests for hyperadrenocorticism are perfect. Imaging can also play a role. Awareness of hyperadrenocorticism has heightened over time. Thus, case presentation is more subtle. Due to the changes in manifestations as well as test technology the Panel believes that references ranges should be reestablished. The role of cortisol precursors and sex hormones in causing a syndrome of occult hyperadrenocorticism remains unclear."
Inoculation of dogs with a recombinant ACTH vaccine. Robert J. Kemppainen. Am.J.Vet.Research. Dec. 2013;74(12):1499-1505. Quote: "Objective: To determine whether inoculation of healthy dogs with a recombinant peptide containing 3 copies of ACTH would result in the production of antibodies against ACTH and whether this would affect pituitary-adrenocortical function. Animals: 8 healthy dogs. Procedures: A recombinant peptide consisting of 3 copies of ACTH fused to a T-helper cell epitope was produced in Escherichia coli. The protein was inoculated into 4 dogs at 4-week intervals (total of 3 inoculations/dog). Four control dogs received inoculations of PBS solution mixed with adjuvant. Blood samples were collected for determination of antibody titers against ACTH and for measurement of basal and ACTH-stimulated plasma cortisol concentrations. Results: Inoculation with the ACTH vaccine resulted in production of anti-ACTH antibodies in all 4 dogs. Titers were initially high but declined by 15 weeks after the initial inoculation. Basal cortisol concentrations were unaffected by inoculation with the ACTH vaccine. Plasma cortisol concentrations in response to ACTH stimulation were reduced at 12 weeks, but not at 15 weeks, after the first inoculation. Conclusions and Clinical Relevance: Inoculation of dogs with a recombinant ACTH vaccine resulted in the production of antibodies against the hormone. Anti-ACTH titers were initially high but were not sustained. The only detectable endocrine effect in treated dogs was a reduction in cortisol concentration in response to ACTH stimulation in 2 of 4 dogs at 12 weeks after the first inoculation. The effect of vaccine administration on the pituitary-adrenal system was subtle and transient."
Canine Cushing’s Syndrome: Some Old but Everything New. Mark E. Peterson. The Animal Endocrine Clinic;NAVC. 2014.
Trilostane for the Treatment of Hyperadrenocorticism: Things Learned Over the Past 10 Years. Doug Brum. MSPCA-Angell. September 2014. Quote: "It is extremely common for serum potassium levels to be elevated when using Trilostane. In fact, you should expect mild to moderate elevations. Given its mechanism of action, this should not be surprising. Trilostane should be used with caution with anti-aldosterone drugs (e.g. ACE inhibitors, spironolactone). Occasionally, one will need to change to a different medication if the potassium rises too high."
Effect of Breed on Plasma Endothelin-1 Concentration, Plasma Renin Activity, and Serum Cortisol Concentration in Healthy Dogs. K. Höglund, A.-S. Lequarré, I. Ljungvall, K. Mc Entee, A.-C. Merveille, M. Wiberg, V. Gouni, J. Lundgren Willesen, S. Hanås, G. Wess, L. Mejer Sørensen, L. Tiret M. Kierczak, S.K.G. Forsberg, E. Seppälä, K. Lindblad-Toh, H. Lohi, V. Chetboul, M. Fredholm, J. Häggström. J. Vet. Intern. Med. January 2016;30:566-573. Quote: Background: There are breed differences in several blood variables in healthy dogs. Objective: Investigate breed variation in plasma endothelin-1 (ET-1) concentration, plasma renin activity, and serum cortisol concentration. Animals: Five-hundred and thirty-one healthy dogs of 9 breeds [including 34 cavalier King Charles spaniels] examined at 5 centers (2-4 breeds/center). Methods: Prospective observational study. Circulating concentrations of ET-1 and cortisol, and renin activity, were measured using commercially available assays. Absence of organ-related or systemic disease was ensured by thorough clinical investigations, including blood pressure measurement, echocardiography, ECG, blood and urine analysis. Results: Median ET-1 concentration was 1.29 (interquartile range [IQR], 0.97-1.82) pg/mL, median cortisol concentration 46.0 (IQR, 29.0-80.8) nmol/L, and median renin activity 0.73 (IQR, 0.48-1.10) ng/mL/h in all dogs. Overall, breed differences were found in ET-1 and cortisol concentrations, and renin activity (P < .0001 for all). Pair-wise comparisons between breeds differed in 67% of comparisons for ET-1, 22% for cortisol, and 19% for renin activity, respectively. Within centers, breed differences were found at 5/5 centers for ET-1, 4/5 centers for cortisol, and 2/5 centers for renin activity. Newfoundlands had highest median ET-1 concentration, 3 times higher than Cavalier King Charles Spaniels, Doberman Pinschers, and Dachshunds. Median renin activity was highest in Dachshunds, twice the median value in Newfoundlands and Boxers. Median cortisol concentration was highest in Finnish Lapphunds, almost 3 times higher than in Boxers. Conclusions and clinical importance: Breed variation might be important to take into consideration when interpreting test results in clinical studies.
Dynamic computed tomography of the pituitary gland using a single slice scanner in dogs with pituitary-dependent hypercortisolism. Sara Del Magno, Guy C.M. Grinwis, George Voorhout, Björn P. Meij. Research in Vet. Sci. May 2016. Quote: Selective removal of the pituitary adenoma has not been advocated in dogs with pituitary-dependent hypercortisolismbecause the pituitary adenoma is usually not visualized on routine computed tomography (CT). Dynamic pituitary CT scanning is aimed at the detection of the pituitary flush and, indirectly, at the presence and position of the adenoma. The first aim of this retrospective study was to compare findings of a multiple slice dynamic scanning protocol with those of a single slice dynamic protocol using a single slice CT scanner. The second aim was to compare the CT findings with surgical findings, and surgical findings with histopathological findings. Computed tomography with single and multiple slice dynamic scanning protocols was performed in 86 dogs with pituitary-dependent hypercortisolism. ... The dogs included 35 different breeds and the most common breeds were Maltese (nine dogs), Dachshund (six dogs), Beagle (six dogs), Cavalier King Charles Spaniel (five dogs), and Jack Russell Terrier (four dogs). There were 31 other breeds (44 dogs) and 12 mixed breed dogs. ... Thirty dogs underwent transsphenoidal hypophysectomy and pituitary specimens were collected as tumor, normal, mixed and neurohypophyseal samples and processed for histology. The pituitary flush was not detected more frequent in multiple slice dynamic scanning series than in single slice dynamic scanning series. However, in non-enlarged pituitaries, the flush was seen significantly more frequently than in enlarged pituitaries. Prediction of the nature of the tissue during hypophysectomy by the surgeon was inconclusive. In conclusion, when using a single slice CT scanner, both single or multiple slice dynamic scanning protocols can be used for localization of the neurohypophyseal flush, and, indirectly, the adenoma. However, based on this study, the aim of surgery in dogs with pituitary-dependent hypercortisolism remains total adenohypophysectomy, and when the neurophypophysis is recognized, it may be left in situ.
Cardiogenic Pulmonary Edema in a Dog Following Initiation of Therapy for Concurrent Hypoadrenocorticism and Hypothyroidism. Jooyae Paik, Ji-Houn Kang, Dongwoo Chang, Mhan-Pyo Yang. JAAHA. September 2016. Quote: A 5-year-old intact female cocker spaniel dog weighing 7.8 kg was referred with anorexia, vomiting, and depression. At referral, the dog was diagnosed initially with typical hypoadrenocorticism, and 2 d later, concurrent primary hypothyroidism was detected. Hormonal replacement therapies, including fludrocortisone, prednisolone, and levothyroxine, were initiated, but a few days later the dog became abruptly tachypneic, and thoracic radiographs indicated the development of pulmonary edema. Echocardiography showed that there were abnormalities indicating impaired left ventricular function, although the heart valves were normal. Following treatment with pimobendan and furosemide, the pulmonary edema resolved. The dog had no recurrence of the clinical signs after 10 mo of follow-up, despite being off all cardiac medications; consequently, the cardiac failure was transient or reversible in this dog. The case report describes the stepwise diagnosis and successful treatment of cardiogenic pulmonary edema after initiation of hormonal replacement therapy for concurrent hypoadrenocorticism and hypothyroidism in a dog.
Evaluation of individual low-dose dexamethasone suppression test patterns in naturally occurring hyperadrenocorticism in dogs. Michael Bennaim, Robert E. Shiel, Christopher Forde, Carmel T. Mooney. J. Vet. Intern. Med. May 2018;32(3):967-977. Quote: Background: Dogs with hyperadrenocorticism (HAC) may be more mildly affected at the time of diagnosis today, which could influence the prevalence of associated clinical and clinicopathological abnormalities and diagnostic test performance. Different low-dose dexamethasone suppression test (LDDST) result patterns have not been evaluated individually. Objectives: To assess the current features of HAC and evaluate if the diagnostic test performance of individual LDDST result patterns differ. Animals: One hundred and twenty-three dogs [including 10 cavalier King Charles spaniels] undergoing investigation for HAC. Methods: Retrospective evaluation of dogs in which a LDDST was performed and HAC confirmed or excluded by alternative means. Cases with basal cortisol concentrations (t0) < 1 μg/dL were excluded. Each LDDST result was classified as (a) complete suppression (t3 and t8<1 μg/dL), (b) lack of suppression (t3 and t8>1 μg/dL and both>50% t0), (c) partial suppression (t3 and t8>1 μg/dL but either<50% t0), (d) escape (t8>1 μg/dL and t3<1 μg/dL) or (e) inverse (t3>1 μg/dL and t8<1 μg/dL) pattern. Results: Fifty-nine (48%) [4 CKCSs] dogs were diagnosed with HAC and 64 (52%) [6 CKCSs] with non-adrenal illness. Hyperadrenocorticism cases had similar clinicopathological abnormalities compared to previous reports. Sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV) (95% confidence interval [CI]) of the LDDST for diagnosing HAC were 96.6 (91.9-100)%, 67.2 (55.7-78.7)%, 73.1 (63.2-82.9)%, and 95.6 (89.5-100)%, respectively. Lack of suppression pattern had the highest PPV (93.9 [85.8-100]%) followed by the partial suppression pattern (67.9 [50.6–85.2]%) and escape or inverse pattern (36.8 [15.1–58.5]%). Conclusions and Clinical Importance: A lack of suppression LDDST pattern has the highest PPV for diagnosing HAC followed by a partial suppression pattern. By contrast, the escape or inverse pattern provided limited support of HAC.
Cushing’s syndrome — an epidemiological study based on a canine population of 21,281 dogs. Gaia Carotenuto, Eleonora Malerba, Costanza Dolfini, Francesca Brugnoli, Pasquale Giannuzzi, Giovanni Semprini, Paolo Tosolin, Federico Fracassi. Open Vet. J. January 2019;9(1):27-32. Quote: The epidemiological characteristics of spontaneous hypercortisolism (HC) were derived from 21,281 client-owned dogs selected from four private veterinary clinics and one university reference center for endocrinology. The odds ratio (OR) method was employed to investigate the risk of developing HC related to breed, gender, and sexual status. The estimated prevalence of HC in the four private clinics was 0.20% [95% confidence interval (CI), 0.13–0.27] and was significantly different compared to the university reference center (1.46%; 95% CI, 1.12–1.80). Sex, breed, and age resulted in risk factors for HC. Mean (± SD) age for dogs with HC was 9.8 (± 2.5) yr. Females had higher risk for HC compared to males (OR 1.85; 95% CI, 1.24–2.75); all neutered dogs (both males and females) had higher risk than intact dogs (OR 2.54; 95% CI, 1.72–3.73); and neutered females had higher risk compared to intact females (OR 2.61; 95% CI, 1.54–4.42). ... Of the 32 different breeds (including the mixed breed category) of dogs with HC admitted to the five clinics over the period of the study, 16 (including the mixed breed category) had at least two dogs with HC and were, therefore, included in the analysis. Using the mixed breed dogs as a control population (OR = 1), the risk of developing HC was significantly higher in the Standard Schnauzer (OR 58.1; p < 0.0001), Fox Terrier (OR 20.33; p < 0.0001), Cavalier King Charles Spaniel (OR 8.03; p < 0.0001), Boxer (OR 7.67; p < 0.0001), ShihTzu (OR 6.56; p = 0.0033), Bolognese (OR 6.30; p < 0.0001), pit bull (OR 5.98; p = 0.0009), Jack Russell Terrier (OR 5.65; p = 0.0081), Maltese (OR 4.90; p = 0.001), Miniature Dachshund (OR 3.52; p = 0.0027), Miniature Poodle (OR 3.44; p = 0.0033), and Yorkshire Terrier (OR 3.43; p = 0.0018). ... With regard to HC, this study identified an overall prevalence of 0.20%. The data support the existence of sex predisposition, with the highest risk for neutered females.
Diagnosis and management of hyperadrenocorticism in dogs attending UK primary-care practice. Imogen Schofield, David Brodbelt, Stijn Niessen, Anna Wilson, Dan O’Neill. BSAVA Congress 2019 Proceedings:437. April 2019. Quote: Objectives: To describe the diagnosis and management of hyperadrenocorticism in dogs attending primary-care practice in the UK. Methods: The VetCompass database contains electronic patient records for dogs attending UK primary-care practices. The records of dogs diagnosed with hyperadrenocorticism were reviewed and additional diagnostic and management data were extracted including: diagnostic testing, treatment, trilostane dose and monitoring cortisol measurements. Results: The study identified 219 dogs diagnosed with hyperadrenocorticism. The most commonly used diagnostic tests were the ACTH stimulation test (n = 206 cases, 94.1%), low-dose dexamethasone suppression test (70, 32.0%) and urine cortisol-creatinine ratio (58, 26.5%). Differentiation between pituitary- and adrenaldependent aetiology was performed in 44 cases (20.1%). Trilostane was given in 206 cases (94.1%) with a mean starting dose of 3.30 mg/kg/day (SD 1.28). Ninety-four cases (45.6%) had no changes made to their initial trilostane dose. Of dogs with cortisol concentrations recorded after initiation of therapy, post-ACTH stimulation cortisol did not drop below the upper reference range of 250 nmol/L in any test in 32 (32.0%) and results fell below the lower reference range of 40 nmol/L in 21 (21.0%). Iatrogenic hypoadrenocorticism or a suspected adverse response was recorded in 28 (13.6%) dogs receiving trilostane. Statement (Conclusions): This study provides benchmark data describing the diagnosis and management of hyperadrenocorticism in primary-care practice. Findings show the ACTH stimulation test predominates in diagnosis and differentiation between pituitary and adrenal disease is infrequently performed, contrary to current expert recommendations. Further work evaluating the benefits of disease differentiation and survival after treatment in a primary-care setting is merited.
Laboratory assessment of trilostane treatment in dogs with pituitary-dependent hyperadrenocorticism. Carolina Arenas Bermejo, Dolores Pérez Alenza, Paula García San José, Lidia Llauet, Laura Pérez-López, Carlos Melián, Edward C. Feldman. J. Vet. Intern. Med. June 2020; doi: 10.1111/jvim.15830. Quote: Background: Results of ACTH stimulation test (ACTHst), pre- and post-trilostane serum cortisol concentrations (SCCs), urine concentration (urine-specific gravity [USG]), and urine cortisol : creatinine ratios (UCCRs) are common variables used to monitor trilostane treatment of dogs with pituitary-dependent hyperadrenocorticism (PDH). However, none has consistently discriminated dogs receiving an adequate dose (A) from those overdosed (O) or underdosed (U). Objectives: To assess and compare recommended monitoring variables, including serial SCCs in a cohort of dogs with PDH treated with trilostane. Animals: Privately owned dogs with PDH (n = 22) and 3 healthy dogs (controls). Methods: Prospective, multicenter, 2-day study. On day “a” (randomized): ACTHst was completed. Day “b” (>2 to <7 days later): SCCs were assessed −0.5 hours, immediately before, and 1, 2, 2.5, 3, 3.5, 4, 6, 8, and 12 hours after trilostane administration. On the first study day, urine collected at home was assessed for USG, UCCR and owner opinions regarding PDH were categorized as: A (clinical signs resolved), U (remains symptomatic), or ill (possible O). Results: At 27 pairs of evaluations, 7 dogs were categorized as A, 19 U, and 1 possible O (excluded from the study). There was overlap in SCC results from the A and U dogs at every time point. Results of USG, UCCR, and ACTHst did not discriminate A from U dogs. Trilostane suppresses SCC within 1 hour of administration and its duration of action in most PDH dogs is <8 hours. Conclusions and Clinical Importance: No single variable or group of variables reliably discriminated A dogs from U dogs during trilostane treatment for PDH.
Frequency and risk factors for naturally occurring Cushing's syndrome in dogs attending UK primary-care practices. I. Schofield, D. C. Brodbelt, S. J. M. Niessen, D. B. Church, R. F. Geddes, D. G. O'Neill. J. Sm. Anim. Pract. December 2021; doi: 10.1111/jsap.13450. Quote: Objectives: To estimate the frequency and risk factors for Cushing's syndrome in dogs under UK primary veterinary care. Materials and Methods: Dogs with Cushing's syndrome were identified by searching electronic patient records of primary-care veterinary practices. Pre-existing and incident cases of Cushing's syndrome during 2016 were included to estimate the 1-year period prevalence. Incident cases were used to estimate the annual incidence and to identify demographic risk factors for the diagnosis of Cushing's syndrome in dogs, through multivariable logistic regression. Results: Analysis included 970 pre-existing and 557 incident cases of Cushing's syndrome from a population of 905,544 dogs. The estimated 1-year period prevalence for Cushing's syndrome in dogs under veterinary care was 0.17% (95% confidence interval 0.16 to 0.18) and incidence was 0.06% (95% confidence interval 0.05 to 0.07). [Cavalier King Charles Spaniel (CKCS) ranked 9th in overall estimated prevalence of Cushing's syndrome in dogs under primary veterinary care in the UK, prevalence 0.19%, with 14 cases.] In multivariable logistic regression modelling, the Bichon frise (odds ratio=6.17, 95% confidence interval 4.22 to 9.00), Border terrier (5.40, 95% confidence interval 3.66 to 7.97) and Miniature schnauzer (3.05, 95% confidence interval 1.67 to 5.57) had the highest odds of Cushing's syndrome. [CKCS ranked 13th (1.24, 95% confidence interval 0.71 to 2.17).] The Golden retriever (0.24, 95% confidence interval 0.06 to 0.98) and Labrador retriever (0.30, 95% confidence interval 0.17 to 0.54) were the most protected breeds. Increasing age, bodyweight greater than the breed-sex mean and being insured also showed increased odds of Cushing's syndrome. Clinical Significance: As Cushing's syndrome is predominately diagnosed and managed in primary-care practice, this study provides valuable new information of its epidemiology in this setting. Demographics reported are supportive of previous work and additional novel associations identified, such as the Border terrier, could enhance the index of suspicion for veterinarians.


CONNECT WITH US