Chronic Ulcerative Paradental Stomatitis (CUPS)
and the Cavalier King Charles Spaniel
What It Is
Cavalier King Charles spaniels are reported to be "over-represented" in contracting a paradental disease called chronic ulcerative paradental stomatitis (CUPS)* or Canine Chronic Ulcerative Stomatitis (CCUS), and the breed may be genetically predisposed to this disease. Maltese terriers also are reportedly over-represented.
CUPS are extremely painful, inflammed sores and ulcers on the soft tissues which come in contact with the teeth (paradental areas**). The are believed to be an allergic response to bacterial plaque on the teeth.
* CUPS is also known as
idiopathic stomatitis, lymphocytic-plasmacytic stomatitis,
contact mucositis, contact mucosal ulceration, and the kissing ulcer.
** "Paradental" refers to soft tissues
which come in contact with teeth, including portions of the oral mucosa,
margins of the lips, and the edges of the tongue. Paradental tissues are
different from periodontal tissues, which are the gums (gingiva) and
harder tissues which support the teeth. CUPS also is different from
eosinophilic stomatitis, which may be very similar in appearance,
since it is an inflammation of the mucous lining of any parts of the
mouth and usually appears as ulcers and lesions on other soft surfaces
within the mouth. Pneumocystis pneumonia is
another disorder to which CKCSs are predisposed and with inflammation in
the mouth, including lesions, as symptoms.
RETURN TO TOP
Symptoms
Since severe mouth pain is a major factor of CUPS, most of the symptoms stem from it. Signs include:
• diffiulty eating
• excessive drooling of thick saliva
• abnormal chewing or refusal to chew or even eat
• pawing at the mouth
• chattering the teeth
• bleeding in the mouth
• inflammed ulcers and reddish areas
• severe halitosis
Mature dogs of any age may be affected.
RETURN TO TOP
Diagnosis
 A
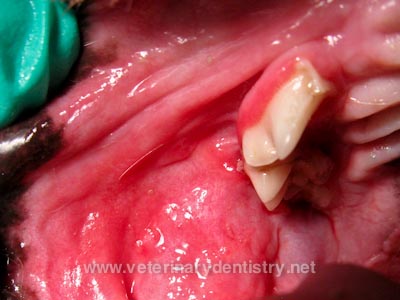
visual examination of the dog's mouth will reveal the ulcers and
inflammed tissues. Since CUPS is presumed to be prompted by bacterial
plaque on the teeth, that will be observed, along with gingivitis and
possible gingival recession around teeth. However, it is not
considered to be infectious. The antigens in bacterial plaque are
suspected to be the stimulants. Inflammed tongue, deep
pocket formations of the gums around teeth, and periodontal bone loss,
and dermititis of the lip folds may also be present. (The photo at
the right is of a CKCS with CUPS, provided by Dr. Brett Beckman at
veterinarydentistry.net.)
A
visual examination of the dog's mouth will reveal the ulcers and
inflammed tissues. Since CUPS is presumed to be prompted by bacterial
plaque on the teeth, that will be observed, along with gingivitis and
possible gingival recession around teeth. However, it is not
considered to be infectious. The antigens in bacterial plaque are
suspected to be the stimulants. Inflammed tongue, deep
pocket formations of the gums around teeth, and periodontal bone loss,
and dermititis of the lip folds may also be present. (The photo at
the right is of a CKCS with CUPS, provided by Dr. Brett Beckman at
veterinarydentistry.net.)
Because the symptoms mimic so many other disorders, it may be necessary to diagnose by routine lab tests, including a complete blood count serum chemistry profile, urinalysis, x-ray, and electrocardiography, to eliminate other possible causes. According to a 2004 study, a laboratory finding commonly associated with CUPS is "hyperproteinemia secondary to a hypergammaglobulinemia (polyclonal) and mild (up to 25,000/ml) neutrophilic leukocytosis."
In a 2017 study, the researchers devised a 32-point Canine Ulcerative Stomatitis Disease Activity Index (CUSDAI) to evaluate the presence of and extent of CUPS in suspected dogs. Categories within CUSDAI include weight loss, pain score, several types and sizes of ulcers, the dog's stage of periodontitis, and bacterial infection.
A definitive diagnosis can only be made by skin biopsies of the lesions, which requires anesthesia. However, the other apparent conditions may enable the veterinarian to presumptively diagnose CUPS without the need for biopsies.
RETURN TO TOP
Treatment
Intial treatment is a thorough cleaning of the dog's teeth, called
dental prophylaxis, which includes removal of all plaque and tartar
(calculus) on the teeth, polishing teeth and extraction of diseased
teeth, and irrigation of the
 gums. Some veterinarians recommend applying
waxy coatings to the teeth, such as
Merial's Ora-Vet, to inhibit future bacterial
growth on the teeth.
gums. Some veterinarians recommend applying
waxy coatings to the teeth, such as
Merial's Ora-Vet, to inhibit future bacterial
growth on the teeth.
The vet probably will prescribe an antibiotic aimed at gram-negative anaerobic bacteria, such as amoxicillin trihydrate-clavulanate potassium, clindamycin, metronidazole*, or a tetracycline. In severe cases, metronidazole or clindamycin may also be dispensed. Some vets may also give prednisone, cyclosporine, or other steroid to suppress the inflammation.
* Metronidazole (Flagyl) may cause adverse events in dogs hypersensitive to it. See Metronidazole Risks.
In a January 2023 article, a team of USA veterinary dental specialists evaluated the effectiveness of a combination of cyclosporine and metronidazole in managing CUPS in ten affected dogs. They were prescribed oral cyclosporine at the rate of 5 mg/kg daily for 1 week, after which they added oral metronidazole at 15-20 mg/kg per day. The cyclosporine dosage interval was lengthened over time. The dogs were observed for a 6-month period and evaluated using the 32-point Canine Ulcerative Stomatitis Disease Activity Index (CUSDAI). They report finding that the combination of cyclosporine and metronidazole was effective in minimizing the clinical signs of CCUS and in reducing CUSDAI scores. They concluded that evaluation of clinical signs and CUSDAI scores appears to be the most effective means of assessing response to therapy, and therapeutic drug level monitoring did not appear to be routinely required.
Thereafter, for the remainder of the dog's life, its teeth must be kept as clean as possible with meticulous home care to avoid any plaque build up. This includes consistent daily brushings, chlorhexidine rinses, and a barrier sealant such as weekly applications of Merial's Ora-Vet or a similar product.
RETURN TO TOP
Research News
February 2016:
Dental specialist Jan Bellows summarizes chronic ulcerative
paradental stomatitis.
 In a
January 2016 article,
Dr.
Jan Bellows (right), a board certified veterinary dentist (AVDC & AVBP)
in Florida, has
summarized the condition known as chronic ulcerative paradental
stomatitis (CUPS) in dogs. He points out that cavalier King Charles
spaniels are among the few breeds which may be genetically
predisposed to the syndrome. He describes it as inflammatory lesions
in the mucous membranes on the inside of the lips, cheeks, palate,
and tongue.
In a
January 2016 article,
Dr.
Jan Bellows (right), a board certified veterinary dentist (AVDC & AVBP)
in Florida, has
summarized the condition known as chronic ulcerative paradental
stomatitis (CUPS) in dogs. He points out that cavalier King Charles
spaniels are among the few breeds which may be genetically
predisposed to the syndrome. He describes it as inflammatory lesions
in the mucous membranes on the inside of the lips, cheeks, palate,
and tongue.
He emphasizes that the syndrome is inflammatory rather than infectious. Clinical signs include marked halitosis, thick, ropy, and occasionally bloody saliva, pain in and around the mouth; and difficulty chewing hard foods and chew toys.
Treatment involves general anesthesia, a tooth-by-tooth examination, including periodontal probing and x-rays, thorough cleaning of the teeth -- above and below the gum line and then polished. Multiple extractions may be necessary. A dental sealant normally is applied during this procedure. Daily plaque-control care must be performed by the pet owners following the initial treatment. Medications may include pentoxdifylline to decrease inflammation, niacinamide, and pain relief. He does not recommend antibiotic therapy. He states that anti-inflammatory medications in control of CUPS may be helpful but are controversial because the cause of the syndrome (plaque and tartar rubbing against the mucosa) is not addressed.
RETURN TO TOP
RETURN TO TOP
Veterinary Resources
Histopathology Of Canine Ulcerative Stomatitis: A Review Of 65 Cases. Jamie G. Anderson, Colin E. Harvey.
Clinical oral pathology, in Veterinary Dentistry Principles and Practice. Wiggs, R.B.; Lobprise, H.B. Lippincott Williams & Wilkins, publishers. 1997; pp 104-139. [The cavalier King Charles spaniel appears to be genetically disposed to canine ulcerative paradental stomatitis.]
Diagnosing and treating chronic ulcerative paradental stomatitis. Carmichael D. Vet.Med. 2004;99:1008-1011. Quote: "Chronic ulcerative paradental stomatitis (CUPS) is a painful condition of dogs with a hallmark lesion of a paradental ulcer, also called a kissing ulcer. Maltese seem to be overrepresented with CUPS, and a familial predisposition has been noted in Cavalier King Charles spaniels. This condition has also been called ulcerative stomatitis, idiopathic stomatitis, and lymphocytic-plasmacytic stomatitis. It causes such severe pain that it is often difficult for owners to provide dental home care, the patient is unwilling to chew, and more dental plaque accumulates, creating a vicious cycle. Although a presumptive diagnosis can be made, histopathologic evaluation is needed for a definitive diagnosis. The differential list includes acute ulcerative stomatitis, systemic lupus erythematosus, uremia, and candidiasis. The treatment plan should include a complete dental prophylaxis. Teeth with advanced-stage periodontal disease should be extracted. A waxy barrier after prophylaxis retards plaque accumulation. The better the level of home care, the fewer drugs needed. A combination of brushing, applying chlorhexidine daily, applying Oravet (Merial) weekly, and instituting long-term intermittent antibiotic therapy should be undertaken to obtain maximal oral hygiene. Prednisone at tapering doses can be used to suppress the inflammation associated with CUPS. If the patient cannot tolerate prednisone, use azathioprine at tapering doses.Owners should be advised that patients with CUPS will most likely need lifetime therapy."
Dental Corner: Diagnosing and treating chronic ulcerative paradental stomatitis. Daniel T. Carmichael. DVM360.com. Dec. 2004. Quote: "Chronic ulcerative paradental stomatitis (CUPS) is a painful condition in dogs that is also known as ulcerative stomatitis, idiopathic stomatitis, and lymphocytic-plasmacytic stomatitis. The hallmark lesion is a paradental, or so-called kissing, ulcer. Patients with CUPS are usually inappetent or anorectic, and the chief complaint from owners is usually fetid halitosis and drooling. CUPS can affect any dog, but Maltese are overrepresented, and a familial predilection has been shown. Cavalier King Charles spaniels also seem to be genetically predisposed. While dogs of any age can be affected, I have rarely seen CUPS in patients under 1 year old."
Focus on: Chronic Ulcerative Paradental Stomatitis aka CUPS. Fraser A. Hale. Toothvet.com January 2008. Quote: "This is one nasty and frustrating condition! As well as being referred to as CUPS, it may also be called ulcerative stomatitis, idiopathic stomatitis and lymphocytic-plasmacytic stomatitis. This multiplicity of labels is a reflection of the lack of solid understanding of the cause(s) of the condition. ... Certain breeds such as Maltese terriers and Cavalier King Charles Spaniels are reported as being over-represented and in my own experience, I would say Greyhounds also seem more susceptible than the general population. That said, I have seen the condition in a wide variety of breeds and sizes."
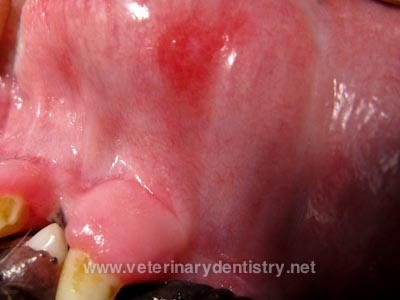 Eosinophilic Stomatitis, Granuloma and CUPS in a Cavalier
King Charles Spaniel. Brett Beckman. veterinarydentistry.net
April 2011. Quote: "This Cavalier had both eosinophilic
stomatitis and CUPS. The CUPS appeared to be the painful component in
this patient and is a consistent component of most if not all cases of
CUPS. Eliminating the plaque with strict home care including brushing
daily, and water additives to reduce plaque (Healthy Mouth) along with
frequent prophy's in the hospital (generally every 3 months) is the
only safe treatment for CUPS. Immuno-suppressive therapy is an
alternative but potentially dangerous approach to therapy. Extracting
the teeth adjacent to the lesions is the only definitive curative
therapy."
Eosinophilic Stomatitis, Granuloma and CUPS in a Cavalier
King Charles Spaniel. Brett Beckman. veterinarydentistry.net
April 2011. Quote: "This Cavalier had both eosinophilic
stomatitis and CUPS. The CUPS appeared to be the painful component in
this patient and is a consistent component of most if not all cases of
CUPS. Eliminating the plaque with strict home care including brushing
daily, and water additives to reduce plaque (Healthy Mouth) along with
frequent prophy's in the hospital (generally every 3 months) is the
only safe treatment for CUPS. Immuno-suppressive therapy is an
alternative but potentially dangerous approach to therapy. Extracting
the teeth adjacent to the lesions is the only definitive curative
therapy."
Chronic Ulcerative Paradental Stomatitis of Dogs. Jan Bellows. Clinicians Brief. January 2016;21-26. Quote: "Chronic ulcerative paradental stomatitis (CUPS)--also known as ulcerative stomatitis, idiopathic stomatitis, lymphocytic plasmacytic stomatitis, and plaque-reactive stomatitis -- is a painful and often debilitating disease involving mucosal areas that contact plaque and calculus in redisposed dogs. Paradental refers to the mucous membranes on the inside of the lips and cheeks, palate, and tongue. The inflammatory lesions do not include the teeth and rarely include the attached gingiva unless accompanied by periodontal disease. The syndrome's appearance results in the term kissing lesions because the injuries are located where the oral mucous membranes rub against the plaque and calculus-laden teeth. Because the syndrome affects companion animals, is usually not chronic or ulcerative, and rarely affects the entire mouth, it was given the name contact mucositis and contact mucosal ulceration by the American Veterinary Dental College (AVDC) in 2013. ... In veterinary practice, affected patients (usually dogs) are generally immune-compromised and develop a hyperimmune mucosal response in the tissues that physically touch plaque. ... Any dog can be affected by contact mucositis. There may be a genetic predisposition to the syndrome, especially in the Maltese dog, greyhound, Cavalier King Charles spaniel, and the Scottish terrier."
Clinical and Histopathologic Characterization of Canine Chronic Ulcerative Stomatitis. J. G. Anderson, S. Peralta, A. Kol, P. H. Kass, B. Murphy. Vet. Pathology. January 2017. Quote: Canine chronic ulcerative stomatitis, also known as chronic ulcerative paradental stomatitis, is a painful condition of the oral cavity. ... Maltese, Cavalier King Charles Spaniel, Labrador Retriever, and Greyhound dogs have a higher reported prevalence. ... The purpose of this study was to determine if there are commonalities in clinical and radiographic features among patients, whether the histopathologic evaluation might inform the pathogenesis, and whether the condition appears similar to human oral mucosal diseases. To do this, we prospectively collected clinical, radiographic, and histopathologic data from 20 dogs diagnosed with the disease. Clinical data were based on a clinical disease activity index, oral and periodontal examination parameters, and full-mouth dental radiographs. The histopathological and immunohistochemical data were based on oral mucosal samples obtained from erosive or ulcerated areas. Our findings revealed that canine chronic stomatitis is clinically characterized by painful oral mucosal ulcers of varying size, pattern, appearance, and distribution, most often associated with teeth with early periodontitis. Histologic examination revealed a subepithelial lichenoid band (interface mucositis) where B cells, T cells, and Forkhead-box protein 3 (FoxP3)- and interleukin-17-expressing cells were present. These cells might play a role in the underlying immune response and an immune-mediated pathogenesis is suspected. The clinical and histopathologic features of this chronic inflammatory mucosal disease in dogs resemble those of oral lichen planus in humans.
Immunopathogenesis of canine chronic ulcerative stomatitis. J. G. Anderson, A. Kol, P. Bizikova, B. P. Stapelton, K. Ford, A. Villarreal, R. J. Jimenez, D. Vasilatis, B. G. Murphy. PLoS ONE. January 2020; doi: 10.1371/journal.pone.0227386. Quote: Canine Chronic Ulcerative Stomatitis is a spontaneously occurring inflammatory disease of the oral mucosa. An immune-mediated pathogenesis is suspected though not yet proven. We have recently reported on the clinical and histologic features, and identification of select leukocyte cell populations within the lesion. A clinical and histologic similarity to oral lichen planus of people was proposed. In the present study, these initial observations are extended by examining lesions from 24 dogs with clinical evidence of chronic ulcerative stomatitis. Because dogs with chronic ulcerative stomatitis often have concurrent periodontal disease, we wondered if dental plaque/biofilm may be a common instigator of inflammation in both lesions. We hypothesized that dogs with chronic ulcerative stomatitis would exhibit a spectrum of pathologic changes and phenotype of infiltrating leukocytes that would inform lesion pathogenesis and that these changes would differ from inflammatory phenotypes in periodontitis. Previously we identified chronic ulcerative stomatitis lesions to be rich in FoxP3+ and IL17+ cells. As such, we suspect that these leukocytes play an important role in lesion pathogenesis. The current study confirms the presence of moderate to large numbers of FoxP3+ T cells and IL17+ cells in all ulcerative stomatitis lesions using confocal immunofluorescence. Interestingly, the majority of IL17+ cells were determined to be non-T cells and IL17+ cell frequencies were negatively correlated with severity on the clinical scoring system. Three histologic subtypes of ulcerative stomatitis were determined; lichenoid, deep stomatitis and granulomatous. Periodontitis lesions, like stomatitis lesions, were B cell and plasma cell rich, but otherwise differed from the stomatitis lesions. Direct immunofluorescence results did not support an autoantibody-mediated autoimmune disease process. This investigation contributes to the body of literature regarding leukocyte involvement in canine idiopathic inflammatory disease pathogenesis.
Medical Management of Canine Chronic Ulcerative Stomatitis Using Cyclosporine and Metronidazole. Kimberly R. Ford, Jamie G. Anderson, Barbara L. Stapleton, Brian G. Murphy, T. K. Santosh Kumar, Todd Archer, Andrew J. Mackin, Robert W. Wills. J. Vet. Dent. January 2023; doi: 10.1177/08987564221148755. Quote: Canine chronic ulcerative stomatitis (CCUS) is a spontaneously occurring, painful, and often debilitating condition of the oral cavity, with a suspected immune-mediated component. The response to pharmacological treatment is generally poor, thus the need to identify more effective medical therapies for this condition. This article describes a prospective clinical trial that was designed to evaluate the efficiency of a combination of cyclosporine and metronidazole in managing CCUS. The hypothesis was that a combination of cyclosporine and metronidazole would effectively minimize clinical signs associated with CCUS. Ten client-owned dogs with a biopsy-confirmed diagnosis consistent with CCUS were prescribed cyclosporine (5 mg/kg) for 1 week, followed by the addition of metronidazole (15-20 mg/kg), both administered orally once daily. The cyclosporine dosage interval was lengthened over time. Dogs were observed for a 6-month period and evaluated using a 32-point Canine Ulcerative Stomatitis Disease Activity Index (CUSDAI). Regular cyclosporine therapeutic drug monitoring was also conducted by the measurement of whole blood cyclosporine levels and the pharmacodynamic assessment of the T-cell expression of IL-2. The results demonstrated that a combination of cyclosporine and metronidazole was effective in minimizing the clinical signs of CCUS and in reducing CUSDAI scores. Neither blood cyclosporine levels nor the T-cell expression of IL-2 predicted improvement in clinical signs and CUSDAI scores, although there was a correlation between blood drug concentrations and the suppression of T-cell IL-2 expression. The evaluation of clinical signs and CUSDAI scores appears to be the most effective means of assessing response to therapy, and therapeutic drug level monitoring does not appear to be routinely indicated.



CONNECT WITH US